The Ordinary Nursery Items That Put 3,500 Babies at Risk Every Year
If You're a New Parent, Stop Using These Nursery Items Immediately
The AAP’s 2022 safe sleep guidelines found that approximately 3,500 infants die annually in the United States from sleep-related deaths—many from hazards hiding in plain sight in nurseries parents thought were safe [1]. This guide shows you the four essential elements of a protective sleep environment and the specific items to remove today.
The nursery looked perfect. Soft cot bumpers to protect her head. A plush mattress so she’d be comfortable. A cozy blanket because the room felt cold. You arranged everything with love.
But here’s what I learned when I studied the research: the safest-looking nursery can be the most dangerous.
When I reviewed the AAP’s 2022 safe sleep recommendations, one number stopped me cold—approximately 3,500 infants die each year in the United States during sleep [1]. Not from rare diseases. From preventable hazards in their sleep environments.
The thing about infant sleep safety isn’t that it’s complicated. It’s that our instincts about what makes babies comfortable often conflict with what keeps their airways open.
Let me show you what actually matters.
Why This Guide Is Different
Evidence-backed and current — Every recommendation comes from the AAP’s 2022 guidelines and peer-reviewed research from 2020-2026, not outdated advice that predates current understanding of SIDS prevention.
Islamic framework woven throughout — This isn’t just a safety checklist. It’s about honoring the amanah (sacred trust) of protecting the life Allah has placed in your hands, with both practical action and prophetic wisdom.
Actionable tools included — You’ll get a free Safe Sleep Environment Setup & Hazard Check (3-page comprehensive PDF) at the end—a room-by-room visual checklist you can use tonight, not just information to remember.
What Makes a Sleep Environment Actually Safe
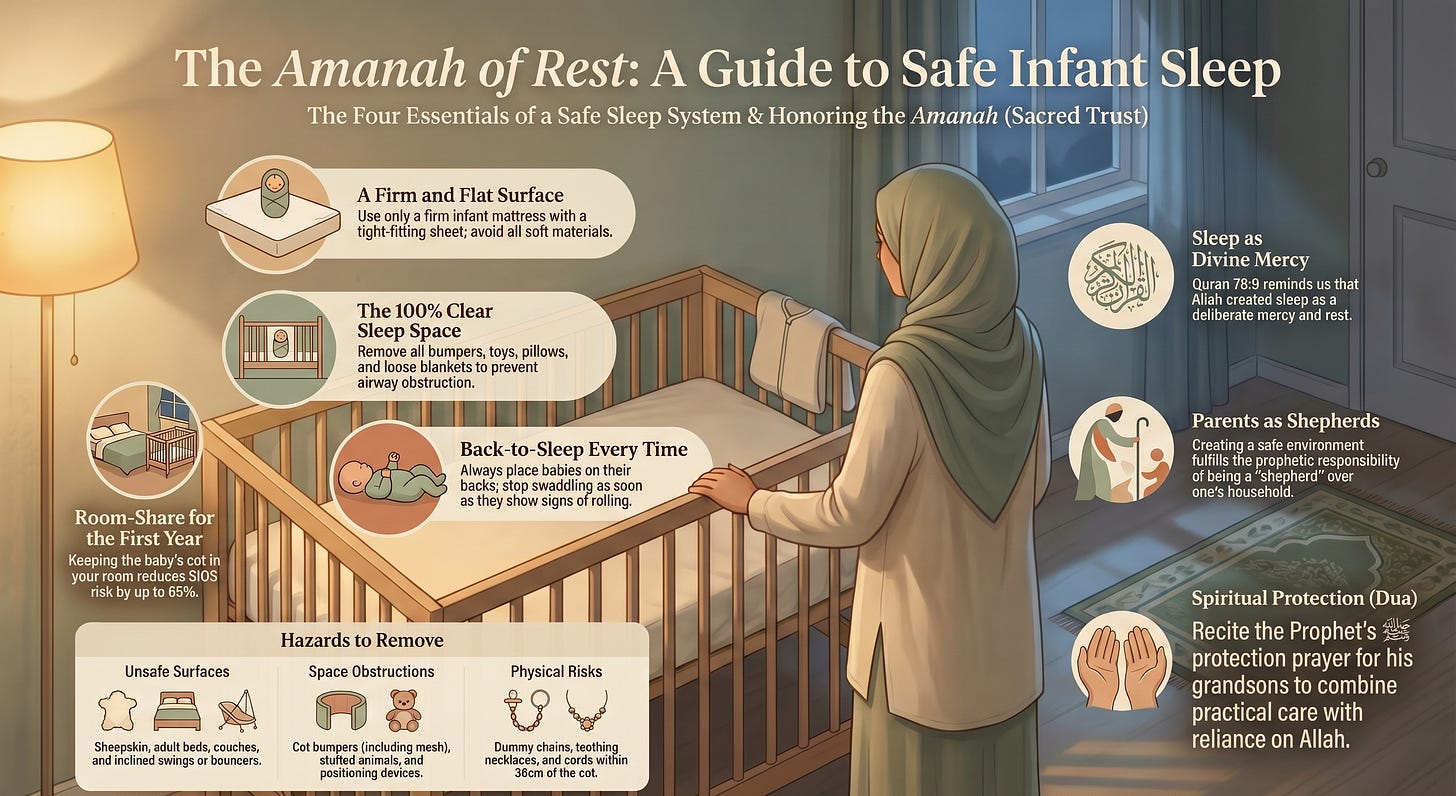
Your baby’s ability to breathe easily during sleep depends entirely on four things working together. Miss one, and the protection fails.
The sleep surface. Firm, flat, and level. Not soft, not inclined, not curved.
The sleep space. Clear of anything that could block airways. Not one soft toy. Not one loose blanket.
The sleep position. On their back. Every single sleep.
The sleep location. In your room. For at least six months, ideally the full first year.
These aren’t suggestions ranked by importance. They’re non-negotiable minimums that work as a system.
But here’s what surprised me when I dug into the research: the biggest risks aren’t the obvious dangers parents worry about. They’re the “comfort items” we add with the best intentions.
The Sleep Surface: Why “Comfortable” Often Means Dangerous
Walk into any baby store and you’ll see them—thick cot mattresses that feel plush, memory foam toppers, sheepskin underlays marketed as “soothing.” They all promise better sleep.
They all compromise your baby’s safety.
When babies sleep on soft surfaces, two things happen that adults don’t experience. First, their faces can sink into the material, creating pockets where exhaled carbon dioxide collects [2]. Second, if they roll onto their stomachs—which starts happening around 3-4 months—they lack the neck strength to lift their heads out of soft bedding [3].
A safe sleep surface is firm enough that when you press your hand into it, it springs back immediately. The mattress should be specifically designed for infants and meet current safety standards [4].
What belongs on that mattress? A tight-fitting fitted sheet over a well-fitted waterproof mattress protector. That’s it.
What doesn’t belong? Anything padded, soft, or cushioned—including mattress toppers marketed as “breathable.” The American Academy of Pediatrics is clear: firm and flat prevents rebreathing [5].
Here’s the category breakdown of unsafe surfaces parents don’t always recognize:
Sheepskin or lamb’s wool underlays (marketed as temperature-regulating)
Adult beds and couches (even without another person)
Pillows, beanbags, or waterbeds used as makeshift sleep spaces
Car seats used for extended sleep outside the car [6]
Any inclined surface, including swings, bouncers, and some rockers
That last one surprises parents. Car seats protect babies during travel, but sleeping at an incline restricts breathing [7]. During long drives, take breaks every two hours to move your baby to a flat surface.
The Sleep Space: The Hazards Hiding in “Safety” Products
This is where it gets tricky. Many products that claim to improve safety actually create new risks.
Cot bumpers top that list.
They’re marketed as protection against head bumps. Research shows they cause deaths through suffocation, strangulation, and entrapment [8]. There’s no safe version—not mesh, not breathable, not thin. Your baby’s cot needs clear sides.
But cot bumpers aren’t the only culprits. I found myself counting hazards in supposedly “safe” nurseries: soft toys “for comfort,” positioning devices “to prevent rolling,” nests and loungers “for better sleep,” weighted sleep sacks “for security.”
Each one blocks airways if your baby’s face makes contact.
Here’s what a truly clear sleep space looks like:
Your baby’s face and head stay uncovered. No hats indoors except in the first hours after birth or in the NICU—they cause rapid overheating [9].
Zero soft objects within reach. No pillows, stuffed animals, cot bumpers, or positioning devices. Parents often add these for emotional comfort (”she looks lonely”), but babies don’t process loneliness the way we do. They process breathing restriction.
Coverings managed carefully. If you use blankets, they must be lightweight, tucked firmly at chest level, with your baby’s feet at the cot bottom so they can’t wriggle down under the blanket [10]. Better option: a properly fitted infant sleep sack with no hood.
No attached items. Teething necklaces, dummy chains, or cords pose strangulation risks [11].
Thirty centimeters of clear space around the cot. No plastic bags, blind cords, mosquito nets, or electrical cords within your baby’s reach [12].
But here’s the thing about sleep space safety: it’s not just about what you remove. It’s about temperature.
Research shows overheating increases SIDS risk, but defining “too hot” is harder than you’d think [13]. Room temperature should stay between 68-72°F (20-22°C) [14]. Your baby should wear no more than one layer beyond what you’re wearing—if you’re comfortable in a t-shirt, your baby needs a onesie plus a sleep sack, not a onesie plus pajamas plus a sleep sack plus a blanket.
Watch for sweating, flushed skin, or a chest that feels hot to touch [15]. Those signal overheating before your baby’s in danger.
I know this feels like a lot to remember when you’re already managing feeds, naps, and everything else. That’s exactly why I created the Safe Sleep Environment Setup & Hazard Check—a visual guide you can use to scan your nursery in five minutes and know you haven’t missed anything. Keep reading to download it at the end.
The Sleep Position: Why “Back to Sleep” Is Non-Negotiable
Your baby’s protective reflexes—swallowing, stirring, waking when airways become blocked—work better on their back than in any other position [16].
When babies sleep on their stomachs or sides, three risks increase:
They’re more likely to rebreathe exhaled air, which contains less oxygen [17]
They have less space around mouth and nose, making airway obstruction easier [18]
Their arousal reflexes don’t trigger as reliably [19]
The research on this is so consistent that “back to sleep” is one of the few universal recommendations across all pediatric organizations worldwide.
But around 3-4 months, your baby will start showing signs they can roll [20]. When that happens, stop swaddling immediately. Your baby needs arms free to push up if they roll onto their stomach.
Once they can roll easily both ways—tummy to back and back to tummy, usually by 4-6 months—keep placing them on their back to start sleep, but let them find their own position [21]. Their neck strength at that point protects them in ways it couldn’t earlier.
The Sleep Location: Why Room Sharing Cuts SIDS Risk by Half
This one surprised me when I first read the data. Sharing a room with your baby—not a bed, but a room—reduces SIDS risk by as much as 50% compared to sleeping in separate rooms [22].
The reason? Your presence affects your baby’s sleep patterns in ways researchers are still mapping. Your sounds, movements, and breathing seem to help regulate your baby’s arousal responses [23].
The safest setup: your baby’s cot or bassinet within arm’s reach of your bed. Close enough to hear them, far enough to maintain separate sleep surfaces.
Room sharing works best for at least the first six months, ideally the full first year [24].
Sleep as Divine Mercy: The Islamic Framework for Infant Safety
When I reflect on how Allah designed sleep, I’m struck by this verse:
“And We have made your sleep as a thing for rest.” (Quran 78:9)
According to Tafsir Ibn Kathir, this verse explains that Allah created sleep as “a cessation of movement in order to attain rest from the frequent repetition and going about in search of livelihood during the day” [25]. Sleep isn’t just biological necessity—it’s deliberate mercy from our Creator.
For our babies, this mercy is even more profound. Their bodies are developing at rates we’ll never experience again. Sleep provides the foundation for that growth.
Creating a safe sleep environment honors Allah’s design. When we ensure our infants can breathe easily during rest, we protect the miracle He’s entrusted to us.
The Prophet ﷺ demonstrated this protective care with his grandsons. Ibn Abbas narrated that the Prophet used to seek Allah’s protection for Al-Hasan and Al-Husayn by reciting:
“U’idhukuma bi kalimat Allah al-tammati min kulli shaytanin wa hammah wa min kulli ‘aynin lammah” — “I seek refuge for you both in the Perfect Words of Allah from every devil and every poisonous pest, and from every harmful eye.” (Sahih al-Bukhari 3371) [26]
He would then say, “Thus Ibrahim used to seek refuge with Allah for Ishaq and Ismail” [27]. This practice teaches us that protection begins with dua and reliance on Allah, even as we implement every physical precaution available.
The hadith also establishes a principle: parents are shepherds over their children. The Prophet ﷺ said, “All of you are shepherds and each of you is responsible for his flock. A man is the shepherd of the members of his household and he is responsible for them” (Sahih al-Bukhari 893) [28].
Creating a safe sleep environment isn’t paranoia. It’s fulfilling the amanah of shepherding the life Allah placed in our care.
Your Safe Sleep Environment Setup & Hazard Check
If you’ve read this far, you’re the kind of parent who takes safety seriously—not as paranoia, but as protective love. That tells me something beautiful about you.
Inside the Safe Sleep Environment Setup & Hazard Check (one comprehensive PDF, 3 pages):
Page 1: Room-by-Room Safety Checklist — A visual walkthrough of every surface, space, and object in your baby’s sleep area, designed as a laminated checklist you can keep by the cot and review weekly as your baby grows.
Page 2: Age-Specific Hazard Guide — What changes at 3 months (rolling signs), 4-6 months (independent rolling), and 6-12 months (standing/climbing)—organized so you know exactly what to watch for and when to make adjustments.
Page 3: Protective Du’as for Infant Sleep — The authentic supplication the Prophet ﷺ used for his grandsons, with Arabic text, transliteration, and translation, plus guidance on when and how to recite it with your baby.
This isn’t just information to file away. It’s a tool designed to stay visible in your nursery—where you’ll actually use it during those moments of doubt at 2 AM when you’re wondering if you remembered everything.
This Safe Sleep Environment Setup & Hazard Check is what every subscriber receives with each article—research-backed guidance you can actually use, rooted in both science and Islamic wisdom.
When you subscribe, you’re joining parents who want more than generic advice.
You’ll receive guidance once its ready. No spam. Just practical guidance you can trust.
The Five-Minute Safety Scan You Can Do Right Now
Don’t wait until you’ve finished setting up the perfect nursery. Walk to your baby’s sleep space right now and check these five things:
Press your hand into the mattress. Does it spring back immediately? (Firm = safe)
Scan the cot. Can you see any soft objects, bumpers, or toys? (Remove them)
Check your baby’s coverings. Are they tucked at chest level with feet at the cot bottom, or is your baby in a sleep sack? (Either works; loose blankets don’t)
Measure the space around the cot. Is there 30 cm of clear space with no cords, bags, or hazards? (Clear = safe)
Feel the room temperature. Are you comfortable in light clothing? (If yes, so is your baby)
Five minutes. Five checks. That’s the difference between wondering if you’re doing it right and knowing you are.
Share This With Someone Who Needs It
Think of a parent you know—maybe your sister who just brought her baby home, your friend who’s pregnant and researching everything, or your neighbor who mentioned feeling overwhelmed by conflicting sleep advice.
Send them this article. Not because they’re doing something wrong, but because having clear, research-backed guidance removes the weight of constant second-guessing.
Frequently Asked Questions About Safe Sleep Environments
Q: Can I use a bassinet or co-sleeper instead of a cot?
Yes, as long as it meets current safety standards for your region. The key requirements: firm, flat surface; well-fitted mattress; no incline; proper ventilation. Bassinets work well for the first few months when room-sharing, then most parents transition to a cot. Just verify it’s not recalled and follows the same rules—no soft bedding, bumpers, or toys inside.
Q: What if my baby seems cold without a blanket?
Your baby needs less warmth than you think. Instead of blankets, use a properly fitted sleep sack (no hood, correct size, appropriate weight for the room temperature). Dress your baby in no more than one layer beyond what you’re wearing. If you’re comfortable in a t-shirt, your baby needs a onesie plus sleep sack—not additional layers. Check for overheating by feeling their chest, not their hands or feet (which naturally run cooler).
Q: When can I add a pillow or stuffed animal for comfort?
Not until after 12 months at the earliest, and many experts recommend waiting even longer. Before age one, these items pose suffocation risks. After the first birthday, SIDS risk drops significantly, but choking and suffocation hazards remain. If you do add a small comfort item after 12 months, keep it tiny (smaller than your baby’s head) and introduce it only when you’re confident your baby can move it away from their face independently. Read the full article section on “The Sleep Space” for details
Q: Is it safe to let my baby sleep in a swing or bouncer for naps?
No. These inclined surfaces restrict breathing and aren’t designed for unsupervised sleep [6]. Use them for awake time only. If your baby falls asleep in one, move them to a firm, flat surface immediately—even if it means waking them partially during the transfer. The breathing restriction risk outweighs the convenience of letting them stay asleep.
Q: What about bed-sharing—is it ever safe?
Bed-sharing carries significant risks and isn’t recommended by the AAP [1]. However, many parents do it—sometimes intentionally, often unintentionally when exhausted. If you find yourself bed-sharing, certain factors dramatically increase danger: smoking, alcohol or drug use, extreme exhaustion, soft bedding, or sharing with anyone other than a biological parent. The safest alternative is room-sharing with separate sleep surfaces. [This topic deserves its own article—watch for our upcoming guide on room-sharing vs. bed-sharing decisions.]
Q: How do I know if the room temperature is right?
The ideal range is 68-72°F (20-22°C) [14]. If you don’t have a thermometer, use this test: if you’re comfortable in light clothing (t-shirt and light pants), the room is probably fine for your baby. Check your baby for signs of overheating—sweating, flushed skin, hot chest, or rapid breathing. These signal you need to remove a layer or lower the room temperature. Your baby’s hands and feet may feel cool even when they’re warm enough, so always check the chest or back of the neck instead.
Q: When can I move my baby to their own room?
The AAP recommends room-sharing for at least the first six months, ideally the full first year [24]. After six months, SIDS risk decreases significantly, but room-sharing continues to offer protection. When you do transition, make sure your baby’s room has the same safe sleep setup—firm surface, clear cot, appropriate temperature—and consider using a video monitor so you can check on them easily.
References
[1] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2022). Sleep-related infant deaths: Updated 2022 recommendations for reducing infant deaths in the sleep environment. Pediatrics, 150(1), e2022057990.
[2] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2005). Policy statement: The changing concept of sudden infant death syndrome: Diagnostic coding shifts, controversies regarding the sleep environment, and new variables to consider reducing risk. Pediatrics, 116, 1245-1255. https://doi.org/10.1542/peds.2005-1499
[3] Moon, R.Y. (2016). SIDS and other sleep-related infant deaths: Evidence base for 2016 updated recommendations for safe infant sleeping environment. Pediatrics, 138(5), Article e20162940. https://doi.org/10.1542/peds.2016-2940
[4] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2011). Policy statement: SIDS and other sleep-related infant deaths: Expansion of recommendations for a safe infant sleeping environment. Pediatrics, 128(5), 1030-1039. https://doi.org/10.1542/peds.2011-2284
[5] Moon, R.Y. (2016). SIDS and other sleep-related infant deaths: Evidence base for 2016 updated recommendations. Pediatrics, 138(5), Article e20162940.
[6] American Academy of Pediatrics, Committee on Fetus & Newborn. (2003). Policy statement: Apnea, sudden infant death syndrome, and home monitoring. Pediatrics, 111, 914-917.
[7] Mannen, E.M. (2019). Biomechanical analysis of inclined sleep products: Final report. College of Medicine, University of Arkansas for Medical Sciences.
[8] Thach, B., Rutherford, G., & Harris, K. (2007). Deaths and injuries attributed to infant crib bumper pads. Journal of Pediatrics, 151(3), 271-277. https://doi.org/10.1016/j.jpeds.2007.04.028
[9] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2022). Sleep-related infant deaths: Updated 2022 recommendations. Pediatrics, 150(1), e2022057990.
[10] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2011). Policy statement: SIDS and other sleep-related infant deaths. Pediatrics, 128(5), 1030-1039.
[11] Moon, R.Y. (2016). SIDS and other sleep-related infant deaths: Evidence base for 2016 updated recommendations. Pediatrics, 138(5), Article e20162940.
[12] Moon, R.Y. (2016). SIDS and other sleep-related infant deaths: Evidence base for 2016 updated recommendations. Pediatrics, 138(5), Article e20162940.
[13] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2022). Sleep-related infant deaths: Updated 2022 recommendations. Pediatrics, 150(1), e2022057990.
[14] National Institutes of Health, Safe to Sleep Campaign. (2026). Ways to reduce baby’s risk. Retrieved from https://safetosleep.nichd.nih.gov/reduce-risk/reduce
[15] National Institutes of Health, Safe to Sleep Campaign. (2026). Ways to reduce baby’s risk.
[16] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2011). Policy statement: SIDS and other sleep-related infant deaths. Pediatrics, 128(5), 1030-1039.
[17] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2005). Policy statement: The changing concept of sudden infant death syndrome. Pediatrics, 116, 1245-1255.
[18] Moon, R.Y. (2016). SIDS and other sleep-related infant deaths: Evidence base for 2016 updated recommendations. Pediatrics, 138(5), Article e20162940.
[19] Moon, R.Y. (2016). SIDS and other sleep-related infant deaths: Evidence base for 2016 updated recommendations. Pediatrics, 138(5), Article e20162940.
[20] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2011). Policy statement: SIDS and other sleep-related infant deaths. Pediatrics, 128(5), 1030-1039.
[21] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2011). Policy statement: SIDS and other sleep-related infant deaths. Pediatrics, 128(5), 1030-1039.
[22] National Institutes of Health, Safe to Sleep Campaign. (2026). Safe sleep environment. Retrieved from https://safetosleep.nichd.nih.gov/reduce-risk/safe-sleep-environment
[23] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2022). Sleep-related infant deaths: Updated 2022 recommendations. Pediatrics, 150(1), e2022057990.
[24] American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome. (2022). Sleep-related infant deaths: Updated 2022 recommendations. Pediatrics, 150(1), e2022057990.
[25] Tafsir Ibn Kathir, commentary on Surah An-Naba (78:9). Retrieved from https://www.alim.org/quran/tafsir/ibn-kathir/surah/78/
[26] Sahih al-Bukhari, Hadith 3371; Sunan Abu Dawud, Hadith 4737; Sunan al-Tirmidhi, Hadith 2060.
[27] Sahih al-Bukhari, Hadith 3371.
[28] Sahih al-Bukhari, Book of Friday Prayer, Hadith 893; Sahih Muslim.